Case Overview
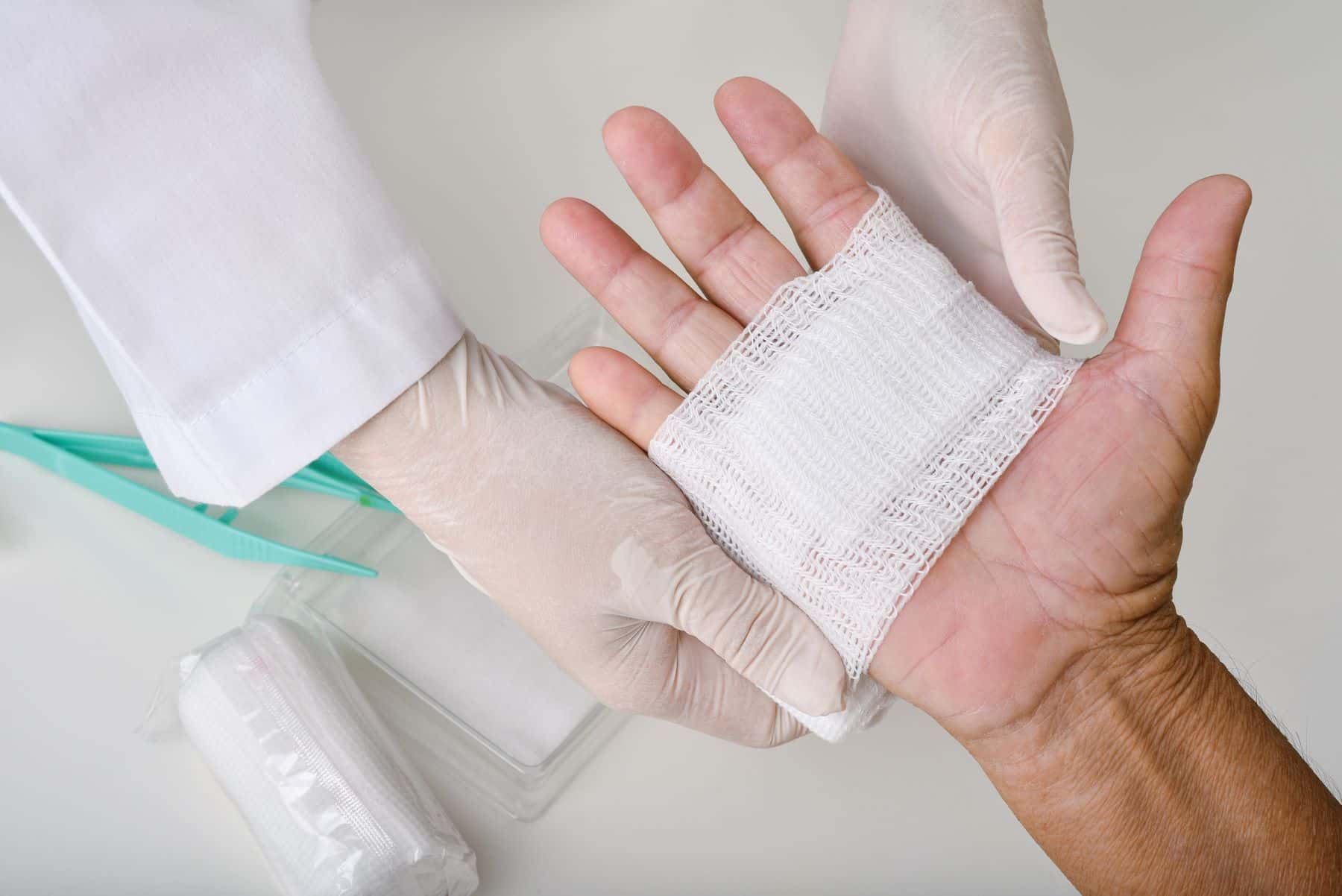
This case study involves a security guard with a history of diabetes mellitus who was assaulted by an individual, resulting in injuries from broken glass to their head, wrist, and ring finger.
The patient sought immediate medical attention in an emergency department. The patient received stitches on their finger and wrist and staples for their scalp wound. However, no oral antibiotics were prescribed upon discharge. The patient was instructed to return after ten days for suture removal.
Tragically, the patient developed a severe infection in their left hand that led to amputation. This case seeks an expert opinion from an experienced emergency medicine physician regarding the standard of care provided.
Questions to the expert and their responses
How often do you treat patients for wrist and hand wounds?
As a board-certified Emergency Medicine physician since 2003, I frequently treat patients with wrist or hand wounds – more than ten times per month.
Generally, what should be done before, during, and after (upon discharge of the patient) when suturing a patient's wrist/hand wound to minimize the risk of infection?
Standard practices include extensive irrigation of the wound prior to suturing and careful examination for any retained foreign body or material within the wound. Prophylactic antibiotics are given if indicated along with a tetanus vaccination if necessary. Sterile technique is crucial during suture repair.
Upon discharge, strict wound care instructions should be provided to the patient including an antibiotic prescription if indicated and close follow-up appointments.
Have you ever reviewed a similar case? If yes, please elaborate.
Yes, I have previously worked on a similar case involving a plaintiff who suffered a hand injury from broken glass. This resulted in permanent function loss.
In addition to my clinical experience, I have held several leadership roles within Emergency Medicine. These include serving as Chief of Emergency Medicine for five years, Director of the Training Lab for the Reanimate Resuscitation Conference for seven years. In addition, I served as QA Director and Education Director for the Department of Emergency Medicine for six and four years respectively. I have also been a member of the Hospital Peer Review Committee for 15 years. I have also been an Expert Reviewer for the Medical Board of California for six years.
About the expert
This expert has an extensive background in emergency medicine, with over 20 years of experience and board certification. They have served in various leadership roles, including Chief of Emergency Medicine at a major hospital and currently as the Director of a Simulation Lab at a resuscitation firm. Their expertise is further highlighted by their current role as an Emergency Medicine Physician at a large trauma center and as the Education Director of an Emergency Department at another hospital.

E-323462
Specialties: